If you’re thinking about dental implants, you may wonder if your jawbone is strong enough to support them.
When you lose a tooth, the bone in that area can shrink over time. Gum disease, injury, or long gaps without teeth can also weaken your jaw.
You need bone grafting before dental implants when your jawbone does not have enough height or width to hold the implant securely.
Without enough bone, the implant may not stay stable, which can lead to failure. A bone graft rebuilds lost bone and creates a solid base for long-term support.
The good news is that not everyone needs a graft. Your dentist checks your bone with exams and 3D scans to see if you have enough support.
Understanding when grafting helps can give you more confidence as you plan your treatment.
Key Takeaways
- Bone loss can occur after tooth loss, gum disease, or injury.
- You may need a bone graft if your jaw cannot securely support an implant.
- A dental exam and imaging help determine the right treatment for you.
Schedule your bone graft consultation in Las Vegas to find out if your jaw is ready for implants.
Understanding Bone Loss and Its Impact on Dental Implants
Bone loss in your jaw can change how stable a dental implant will be. The amount and quality of bone you have affects healing, long‑term support, and your risk of implant failure.
Causes of Jawbone Loss
Your jawbone needs regular pressure from chewing to stay strong. When you lose a tooth, that pressure stops, and the body begins bone resorption, which slowly shrinks the bone in that area.
Other common causes include:
- Gum disease (periodontitis) that damages bone around teeth
- Untreated infections or abscesses
- Injury to the jaw
- Long-term missing teeth
- Smoking and certain medical conditions
Research on bone loss-related factors in dental implants shows that smoking, plaque buildup, and inflammation around implants can also lead to more bone loss after placement.
Jawbone loss can start within months after a tooth is removed. The longer you wait to replace a tooth, the more bone you may lose.
Effects of Bone Loss on Implant Success
Dental implants need solid bone for support. If you do not have enough height or width of bone, the implant may not bond well during healing.
Low bone volume can lead to:
- Poor initial stability
- Delayed healing
- Higher risk of implant failure
Studies often define early failure as more than 1 mm of bone loss in the first year and more than 0.2 mm each year after that, as noted in this review of factors affecting bone loss in dental implants.
If bone loss continues after placement, the implant can loosen. You may also notice gum recession or discomfort when chewing.
Bone Resorption and Bone Density Considerations
Bone resorption is a natural process, but it becomes a problem when it reduces bone density and volume too much.
Dental implants rely on a process called osseointegration, where bone grows tightly around the implant surface.
For this to work, you need:
| Factor | Why It Matters |
| Adequate bone height | Supports implant length |
| Adequate bone width | Prevents exposure of threads |
| Good bone density | Improves stability during healing |
Lower bone density, which is common in the upper jaw or in people with osteoporosis, can reduce implant success rates.
In these cases, your dentist may suggest bone grafting to rebuild the area before placing the implant.
Strong, healthy bone gives your implant the best chance to last for many years.
Assessing the Need for Bone Grafting Before Implant Placement
Before you move forward with a dental implant, your dentist must check if your jaw has enough bone volume to hold it securely.
They use exams and detailed scans to measure bone height, width, and density and decide if a bone graft before implant placement makes sense.
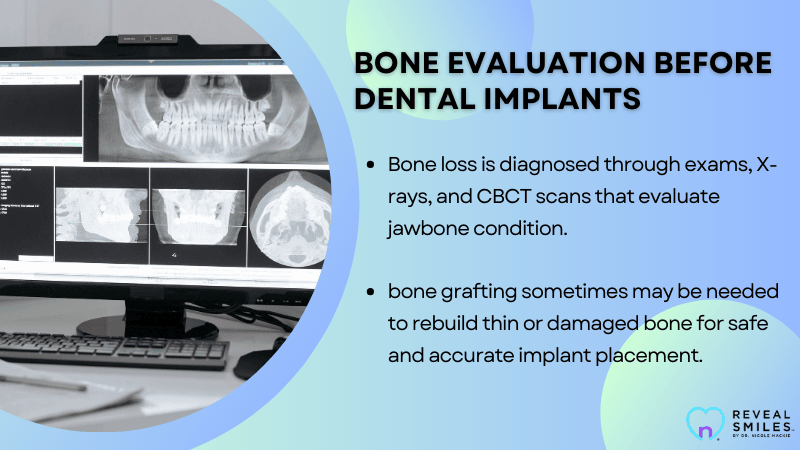
How Bone Loss Is Diagnosed
Your dentist starts with a clinical exam. They look at the shape of your gums and feel the ridge where the tooth is missing.
If the ridge feels thin or looks sunken, you may have lost bone. Long-term tooth loss, gum disease, or trauma often cause this problem.
X-rays give a basic view, but they do not show the full picture. Many offices now rely on advanced scans to measure the exact height and width of your jaw.
Your dentist also reviews your health history. Conditions like uncontrolled diabetes or smoking can affect healing after a dental bone graft.
A careful exam helps your provider decide if you have enough bone to place an implant safely or if you need bone grafting first.
When Bone Grafting Is Recommended
You need bone grafting when your jaw cannot hold an implant firmly. An implant must bond tightly with your natural bone to stay stable.
Your dentist may suggest a bone graft before implant placement if you have:
- A narrow or thin ridge
- Low bone height near the sinus
- Bone damage from gum disease
- Bone shrinkage after years without a tooth
In the upper back jaw, bone loss often occurs near the sinus. In these cases, a sinus lift may add bone height.
Some patients with mild loss may qualify for short or narrow implants. But if bone volume falls below safe limits, a dental bone graft creates a stronger base and lowers the risk of implant failure.
Role of 3D Imaging and CBCT Scans
Modern implant planning depends on 3D imaging. Traditional X-rays show flat images, but they cannot measure bone depth accurately.
Cone beam computed tomography (CBCT) produces a three-dimensional view of your jaw. This scan shows bone width, height, and density in exact detail.
With CBCT, your dentist can see nearby nerves and sinuses. That reduces the risk of complications during surgery.
Many practices explain this process in detail when discussing when bone grafting is necessary before dental implants.
Clear imaging helps you understand why a bone graft before implant placement may improve safety and long-term stability.
Accurate measurements allow for precise implant placement and better healing after bone grafting.
Book your implant assessment today to see if bone grafting is right for you.
Types of Bone Grafts for Dental Implants
Dentists use several types of bone grafts to rebuild your jaw before placing an implant. The right choice depends on how much bone you lost, your health, and how stable the implant site must be.
Autograft and Autografts
An autograft uses bone taken from your own body. Your dentist or oral surgeon may collect it from your chin, jaw, or sometimes your hip.
Because the bone comes from you, it contains living cells that help form new bone. It also has natural growth factors that support healing. This makes autografts strong in bone regeneration.
However, autografts require a second surgical site. That means you may have more swelling, discomfort, and longer surgery time.
You may need this option if you have severe bone loss or need a large amount of bone. Many providers still consider it a reliable choice when your goal is strong bone growth and implant stability.
Allograft and Allografts
An allograft uses donor bone from another person. Tissue banks carefully screen and process this bone to make it safe.
Processing removes living cells, so the graft mainly acts as a scaffold. Your body grows new bone into this structure over time. It does not require a second surgery site, which makes the procedure simpler for you.
Many dentists use allografts for moderate bone loss. They often place them during socket preservation after tooth removal or before implant placement.
The material helps maintain shape and volume while your body heals.
Xenograft and Xenografts
A xenograft uses bone from an animal, most often cow bone. Manufacturers clean and process the material to remove organic parts, leaving a mineral structure.
This structure works as a long-lasting scaffold. Your body slowly replaces it with your own bone, but the material resorbs more slowly than many other grafts.
Dentists often choose xenografts when they need to maintain space and shape. For example, they may use them in sinus lifts or ridge augmentation.
The slow breakdown can help support the area while healing takes place.
This type of graft does not require a second surgical site. You avoid donor site pain, but healing may take several months before your dentist can place the implant.
Synthetic Options: Alloplast
An alloplast is a fully synthetic bone graft. It does not come from you or a donor bone. Common materials include calcium phosphate, beta‑tricalcium phosphate, and bioactive glass.
These grafts act as a framework for new bone growth. Your body gradually replaces the material as healing continues.
Many dentists use alloplasts for small to moderate defects. They are also common in socket preservation and guided bone regeneration.
Some modern materials perform well in selected cases, especially when the goal is to hold space during healing.
Bone Grafting Procedures and Techniques
Dentists and oral surgeons use different bone grafting techniques based on how much bone you have lost and where the implant will go.
Some procedures rebuild large areas, while others fix small defects at the time of implant placement.
Ridge Augmentation
You may need ridge augmentation when your jaw has lost width or height after a tooth has been missing for a long time.
Bone shrinks over time, and this can leave the ridge too thin to hold an implant securely.
During this oral surgery, your oral surgeon places bone graft material along the weak area of the jaw. They may use your own bone, donor bone, animal-based material, or a synthetic option.
In some cases, they secure a small block of bone with tiny screws to rebuild the shape of your jaw.
Healing usually takes several months. The new bone must fuse with your natural bone before implant placement.
Sinus Lift for Upper Jaw Implants
If you need implants in your upper back jaw, you may require a sinus lift. The upper molar area often lacks enough bone because the sinus cavity sits just above it.
In this advanced bone grafting procedure, your oral surgeon gently lifts the sinus membrane upward. They then place bone graft material into the space between your jaw and the sinus floor.
This added bone creates enough height to hold an implant securely. Healing often takes four to nine months before your dentist places the implant.
Minor Bone Graft Procedures
You may only need a minor bone graft if the bone loss is small and limited to one area. Dentists often perform these procedures at the same time as implant placement.
One common method is socket preservation. After a tooth extraction, your dentist places graft material into the empty socket to reduce bone shrinkage.
Another approach is guided bone regeneration. Your dentist places graft material and covers it with a protective membrane to keep soft tissue from growing into the space.
These smaller bone grafting techniques support healing and improve implant stability.
Bone Grafting Recovery and Long-Term Implant Stability
Healing after a bone graft takes time and careful habits. Your actions during recovery directly affect bone regeneration, osseointegration, and long-term implant stability.
What to Expect During Bone Graft Recovery
Right after surgery, you can expect mild swelling, soreness, and minor bleeding. Most symptoms improve within a few days.
Your dentist may place stitches to protect the graft. The area needs time to form new bone cells and connect with the graft material. This process is part of natural bone regeneration.
Healing often takes 3 to 6 months, depending on the size and location of the graft. Larger grafts may need more time before implant placement.
To protect the site, you should:
- Avoid chewing on the grafted side
- Eat soft foods for several days
- Keep the area clean without brushing directly over stitches
- Take prescribed medications as directed
Implant Stability and Osseointegration
After your graft heals, your dentist places the dental implant into the rebuilt bone. At this stage, osseointegration becomes critical.
Osseointegration means your jawbone grows around the implant and bonds to it. This bond creates implant stability and allows the implant to function like a natural tooth root.
Without strong bone support, implants can loosen.
Studies on bone loss-related factors in tissue and bone level dental implants show that bone quality and proper placement affect long-term results.
Osseointegration usually takes a few months. During this time, you must avoid heavy pressure on the implant. Stable bone and careful healing improve long-term implant stability.
Supporting Bone Regeneration for Implant Success
Your daily habits directly affect bone regeneration and implant stability.
Smoking slows healing and reduces blood flow to the graft. Poor oral hygiene can cause infection and bone loss around the implant.
To support healing, you should:
- Brush and floss gently but consistently
- Attend all follow-up visits
- Manage gum disease early
- Maintain a balanced diet with enough calcium and protein
Bone grafting rebuilds lost structure and prepares your jaw for implants.
When you protect the graft and follow care instructions, you give your implant the best chance to stay stable for many years.
The Importance of Professional Consultation and Personalized Care
You need clear answers before you move forward with implant treatment. A detailed exam helps you understand if you need bone grafting and how to plan safe implant placement.
Choosing the Right Treatment Plan
Your dentist or oral surgeon will study your jawbone with digital X-rays or a 3D scan. These images show bone height, width, and density.
They help decide if your bone can hold an implant or if grafting will improve stability.
You may learn that bone grafting is the safest option when bone loss affects long-term results.
Your treatment plan may include:
- Immediate implant placement
- Delayed implant placement after healing
- Bone grafting before or during implant surgery
- Use of short or narrow implants in mild bone loss
Your health history also matters. Conditions like diabetes, smoking, or gum disease can affect healing. A personalized plan lowers risk and improves long-term stability.
Scheduling a Consultation With an Oral Surgeon

When you schedule a consultation, you get a clear review of your bone health and treatment options. The surgeon will examine your mouth, review scans, and explain each step in simple terms.
You should expect a discussion about timing, cost, healing periods, and how implant placement will work in your case.
If bone grafting is needed, your surgeon will explain the type of graft and the recovery timeline.
Bring a list of questions. Ask about:
- Healing time before implant placement
- Risks and possible side effects
- Steps you should take before surgery
- Follow-up visits after the procedure
Clear communication helps you feel prepared and confident about your care.
Frequently Asked Questions
Bone grafting helps rebuild jawbone that has shrunk after tooth loss or gum disease. Healing time, graft type, and your current bone level all affect when and how you can move forward with dental implants.
What are the signs that I might need a bone graft for a dental implant?
You may need a bone graft if your dentist sees bone loss on X-rays or a 3D scan. This often happens after you lose a tooth and wait several months or years to replace it.
Loose dentures, shifting teeth, or advanced gum disease can also point to weak jawbone.
In many cases, providers recommend grafting to create a stable base for implants, as explained in this overview of dental bone grafting for implants.
Can dental implants be successful without sufficient bone density?
Dental implants need enough bone to hold them firmly in place. Without strong bone, the implant may fail to bond with your jaw.
In some cases, mild bone loss may not require grafting.
Your dentist will measure bone height and width before making a decision.
How long does the bone grafting healing process take before getting an implant?
Initial recovery from a bone graft usually takes about a week. The grafted bone, however, needs more time to fully heal and bond with your jaw.
Most small grafts take at least three months to heal. Larger grafts may take nine to 12 months.
Your dentist will confirm healing with imaging before placing the implant.
What are the different types of bone grafts used for dental implants?
Dentists use several types of bone graft materials. These include bone taken from your own body, donor bone, animal bone, or synthetic materials.
Each type works to add volume and density to your jaw.
Your provider will choose the best option based on your health and the size of the defect.
How can I tell if my jawbone is strong enough to support dental implants?
You cannot judge bone strength by looking in the mirror. Your dentist must take digital X-rays or a cone beam CT scan to measure bone thickness and height.
They will check for enough bone to fully cover and support the implant.
A full exam gives you a clear answer before surgery begins.
Are there alternatives to bone grafting if I want to get dental implants?
Some patients qualify for shorter or narrower implants that require less bone. Others may benefit from angled implants or special techniques like sinus lifts, depending on the area of the mouth.
These options depend on your specific bone level and anatomy. Your dentist will review all choices with you so you can decide what fits your goals and health needs.

